CERVICO
VAGINAL CYTOLOGY - CLASSIFICATION WITH A MATHEMATICAL
MODEL
César T.
VELA-VELASQUEZ
1996
To the Editors:
The ideal point of the cytologic diagnosis is that it
is identical to the hystologic diagnosis, that is to
say, with the participation of cytology or histology
we reach the same diagnosis, but in regard to the cytologic
diagnosis we only rely on cellular morphology; however,
we have not taken into consideration important pieces
of information such as: the behavior of the cell with
relation to its same tissue, its behavior with other
neighboring hystologic structures.
Acording to this, we observe in the daily practice that
the cytologic diagnosis has an "indeterminate area"
in relation to the hystologic diagnosis, it is for that
reason that we believe that for the cytologic diagnosis
we have to accept "area of indeterminant cells".
The main objective of the cervical-vaginal cytology
is the detection of neoplastic cells, in which the specification
of dysplasia or carcinoma is considered to be important,
since the first one reflects reversible chromosomal
changes or potentially reversible changes; on the other
hand, in the cancerous cells the chromosomal changes
are irreversible and they acquire infiltration properties
and cellular destruction concomitantly.
In the routine work we frequently have the doubt that
the cellular changes which we observe are due to reactive
changes or if they are dysplasia or cancer; for this
reason, we think that in these 3 categories the problem
of identification of the cellular alterations is located
in the cervical-vaginal cytology. Therefore, it is important
to schematize the universe of the cytologic diagnosis
using a mathematical diagram of the group theory in
the following way:
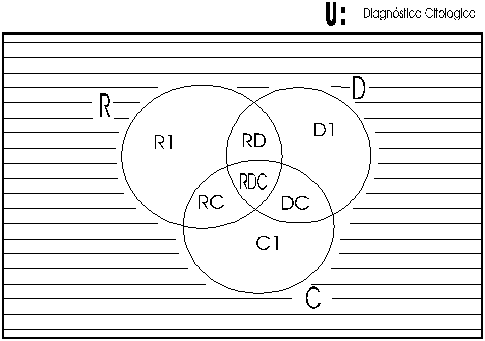
Where:
U: It represents the universe
of all of the cytologic diagnoses.
Group R: All cells in this group
have characteristics consistent with reactive cells.
Group D: All cells in this group
have characteristics consistent with cellular dysplasia.
Group C: All cells in this group
have characteristics consistent with carcinoma.
Area R1: Cells whose characteristics
are undoubtedly of reactive cells.
Area D1: Cells whose characteristics
are undoubtedly of cellular dysplasia.
Area C1: Cells whose characteristics
are undoubtedly of carcinoma.
.............The intersection
areas represent "area of indeterminant cells",
that is, they can
.............correspond
to any of the implied groups, as explained below:
Area RD: Cells with some characteristics
of reactive cells or dysplasia;
Area DC: Cells with
some characteristics of dysplasia or carcinoma;
Area RC: Cells with some characteristics
of reactive cells or carcinoma; and
Area RDC: Cells with some characteristics
of reactive cells or dysplasia or carcinoma.
Finally, the shady area represents the rest of the cytologic
diagnoses.
The size of the morphologic "area of indeterminant
cells" varies according to the population, that
is to say, in some of them it will be small and in others
it will be big, but the important thing is to conceive
these areas because we have the opinion that they will
always exist, since if in the near future many of these
cells will be classified in the correct category with
genetic methods, then it is possible that the cellular
indeterminacy will reside in finer molecular changes,
that is, we want to stress that there will always be
"area of indeterminant cells" until, at any
moment in the future, the evolution of cytology
will be such that these "area of indeterminant
cells" will be equal to zero.
In the cytologic report, we have to get to the ideal
point of balance between our cytologic diagnosis and
the message that has to be given to the patient appropriately,
that is, to make it in such a way that we harm the patient
neither physically nor psychologically, especially when
we refer to these "area of indeterminant cells";
therefore, we have to transfer our message in such a
way that the patient does not neglect her treatment
nor does she feel unquiet (for example
as we will see later, we suggest labeling the area RD
"indeterminant (squamous or glandular) cell with
dyskaryosis", since all dysplastic cells have dyskaryosis,
but not all cells with dyskaryosis are dysplastic; the
same happens to area RC and area RDC, where we only
use the word "neoplasm" and not "malignant
neoplasm", since it is likely to be a reactive
change only).
Consequently, we consider the following terminology
appropriate for the "area of indeterminant cells":
Area RD: Indeterminant (squamous or
glandular) cell with dyskaryosis.
Area RC: Indeterminant (squamous or
glandular) cell of low grade of suspicion of neoplasm.
Area RDC: Indeterminant (squamous or
glandular) cell of high grade of suspicion of neoplasm.
Area DC: Indeterminant
neoplasic (squamous or glandular) cell.
In relation to dysplasia, we believe that it is important
to remember that the exocervical epithelium is the product
of the maturation of the basal cells, and the strange
agent that can produce dysplasia is probably present
already from the basal layer, but the morphologic manifestation
is in the other layers (the more
superficial the squamous cell is, the more
nuclear physiologic mechanisms are lost, that is to
say, the more superficial the cell is, the more sensitive
it becomes, and therefore it may get attacked easily
by strange agents, which can cause chromosomal imbalance),
that is, if we find a superficial cell with dyskaryosis
of dysplasia we speak of mild dysplasia. If it is an
intermediate cell, then it is moderate dysplasia. And
finally, if the dyskaryosis of dysplasia is also in
parabasal cells, we speak of severe dysplasia.
A lot of information on the human papillomavirus (HPV)
has come about; the article written by Richart et al.
(1) is very interesting and complete; we think that
if it is true that the gene of the HPV is already acting
molecularly in the nucleus of the guest cell, while
there is no dyskaryosis evidence it should not be spoken
of dysplasia, since while there is no morphologic manifestation
of nuclear alteration it means that the mechanisms of
genetic protection and the working of the virus is in
a point of balance that makes the cell stay physiologically
normal, but it requires the patient's strict medical
care. The same previous reasoning can be applied in
the future for any element " X " (given by
the cytologic investigation) that can lead to dysplasia
or cancer, that is, if there is no morphologic evidence
of dyskaryosis it should not be spoken of dysplasia.
We believe that the contribution of the Bethesda System
(2), regarding the approach of adecuacy of the sample
and the use of appropriate recommendations in the cytologic
report, is significant; we also believe that the cytologic
report should keep a scientific format, that is, to
give the most comprehensive information with the minimum
number of words.
In conclusion, we suggest that the classification of the
cervical-vaginal cytology be in the following way:
1- NEGATIVE
CYTOLOGY FOR NEOPLASTIC CELL
1.1- Without significant cellular
changes
1.2- With inflammatory pathology
1.2.1- Bacterial cervical-vagintis
(3)
1.2.2- Trichomoniasis
1.2.3- Candidiasis
1.2.4- Cervical infections by Chlamydia (4)
1.2.5- Viral infections (not included the HPV nor
the genital Herpes)
1.2.6- Other inflammatory agents
1.3- With reactive epithelial changes (squamous metaplastic
cells, repair cells, etc.; in generalin association
with inflammatory pathology)
1.4- Cytology with the presence of high-risk agents
(HPV, genital Herpes, other agents given in the future
by the cytologic investigation)
1.5- Hormonal evaluation (the same as the Bethesda
System)
2- CYTOLOGY
WITH INDETERMINANT EPITHELIAL CELLULAR CHANGES:
2.1- Indeterminant (squamous or glandular)
cell with dyskaryosis.
2.2- Indeterminant (squamous or glandular) cell of low
grade of neoplasm suspicion.
2.3- Indeterminant (squamous or glandular) cell of high
grade of neoplasm suspición (for example cell
of "atypical parakeratosis" [5]).
2.4- Indeterminant neoplasic (squamous or glandular)
cell.
3- NEOPLASIC
CYTOLOGY:
3.1- Epithelial cell with cellular
dysplasia:
3.1.1- Mild dysplasia of squamous cell
3.1.2- Moderate dysplasia of squamous cell
3.1.3- Severe dysplasia of squamous cell
3.1.4- Dysplasia of glandular cell
3.2- Cells of malignant neoplasms:
3.2.1-Carcinoma of squamous cells: Optional categories
for differentiations in:
3.2.1.1- Carcinoma in situ
3.2.1.2- Microinvasive carcinoma
3.2.1.3- Invasive carcinoma
3.2.2- Adenocarcinoma
3.2.2.1- Adenocarcinoma of endocervix
3.2.2.2- Adenocarcinoma of endometrium
3.2.3- Other malignant neoplasm:
Specify
Finally, we are convinced that the present article will
contribute in the discussion and classification of the
cervical-vaginal cytology.
REFERENCES
1.Richart
RM, Masood S, Syrjänen KJ, Vassilakos P, Kaufman
RH, Meisels A, Olszewski WT, Sakamoto A, Stoler MH,
Vooijs P, Wilbur DC: Human Papillomavirus. IAC Task
Force Summary.
Acta Cytol 1998;
42: 50-58
2.The
Bethesda System for Reporting Cervical/Vaginal Cytologic
Diagnoses.
Acta Cytol 1993;
37: 115-124
3.Vela
CT, Mendoza N: Diagnóstico citológico
y gram de la vaginosis bacteriana.
Rev Med IPSS 1995;
4: 53-58
4.Vela
CT: Cytologic Diagnosis of Chlamydia in Cervical-vaginal
Secretions. Use of a Papanicolaou Stain Modification
with Buffered Wright Solution.
Acta Cytol 1998;
42: 954-958
5.Vela
CT: "Atypical Parakeratosis" Cells in Cervical
Carcinoma Cytology.
Acta Cytol 1997;
41: 614-616
Acknowlegements:
My gratitude to Mr. Felipe A. Vela-Izquierdo for his
assistance in the translation of the present manuscript.
|


